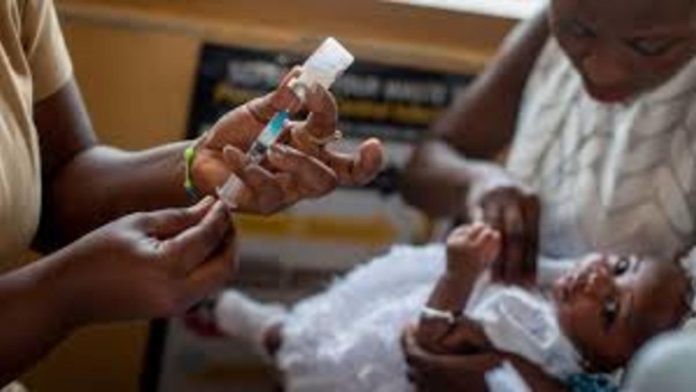
The World Health Organization (WHO) has endorsed the world’s first malaria vaccine and recommended that it be used on African youngsters.
After its expert advisory committees recommended administering the malaria vaccine, WHO Director-General Tedros Adhanom Ghebreyesus issued the decision on Wednesday, calling it “a historic occasion.”
The RTS,S, or Mosquirix, was created in 1987 by GlaxoSmithKline (GSK), a British pharmaceutical company. It has been in development for more than 30 years and is the only known vaccine that has proved to lessen the risk of developing malaria.
“Today’s recommendation offers a glimmer of hope for the continent, which shoulders the heaviest burden of the disease. And we expect many more African children to be protected from malaria and grow into healthy adults,” said Dr. Matshidiso Moeti, WHO’s Africa director.
Mosquirix trials in Africa
Since 2019, WHO has been coordinating Mosquirix research in Ghana, Kenya, and Malawai, with over 8 lakh children receiving the malaria vaccine. Mosquirix has been given to the children in 2.3 million doses so far.
WHO stated its decision was largely based on the findings of continuing study in Ghana, Kenya, and Malawi, where the malaria vaccine has been given to over 800,000 children since 2019.
“This is an African vaccine created by African experts, and we’re quite proud of it,” WHO Director-General Tedros Adhanom Ghebreyesus said.
Mosquirix is the first vaccine to be approved, but it has certain drawbacks: it is only approximately 30% effective, takes up to four doses, and its protection wears out after a few months.
Despite this, scientists believe the vaccine could have a significant impact given the enormous burden of malaria in Africa, which accounts for the majority of the world’s more than 200 million cases and 400,000 fatalities each year.
Julian Rayner, head of the Cambridge Institute for Medical Research, who was not involved in the WHO decision, remarked, “This represents a big step forward.”
“It’s a flawed vaccination, but it will save the lives of hundreds of thousands of children.”
Rayner said the vaccine’s impact on the spread of the mosquito-borne disease was still unclear, but pointed to coronavirus vaccines as an encouraging example.
“The last two years have given us a very nuanced understanding of how important vaccines are in saving lives and reducing hospitalizations, even if they don’t directly reduce transmission,” he said.
Malaria in Africa
Because malaria is a parasitic disease spread by mosquitoes, Dr. Alejandro Cravioto, chair of the WHO vaccine group that issued the recommendation, said creating a vaccine against it was extremely tough.
“We’re confronted with extraordinarily complex organisms,” he said. “We are not yet in reach of a highly efficacious vaccine, but what we have now is a vaccine that can be deployed and that is safe.”
According to the WHO, adverse effects were uncommon, but they did occasionally include a fever that could lead to brief convulsions.
The vaccine, according to Sian Clarke, co-director of the Malaria Centre at the London School of Hygiene and Tropical Medicine, would be a helpful supplement to other anti-malaria techniques that may have outlived their usefulness after decades of usage, such as bed nets and pesticides.
“In some countries where it gets really hot, children just sleep outside, so they can’t be protected by a bed net,” Clarke explained. “So obviously if they’ve been vaccinated, they will still be protected.”
Clarke went on to say that little progress has been achieved against malaria in the last few years.
“If we’re going to decrease the disease burden now, we need something else,” she explained.
According to Azra Ghani, head of infectious diseases at Imperial College London, the introduction of the malaria vaccine in African children could result in a 30% drop in overall infections, with up to 8 million fewer cases and up to 40,000 fewer fatalities per year.
“For people not living in malaria countries, a 30 per cent reduction might not sound like much. But for the people living in those areas, malaria is one of their top concerns,” Ghani said.
“A 30 per cent reduction will save a lot of lives and will save mothers (from) bringing in their children to health centers and swamping the health system.” She expressed hope that the WHO guidance would be a “starting step” toward better malaria vaccines. Ghani believes that the messenger RNA technology employed in two of the most successful COVID-19 vaccines, those from Pfizer-BioNTech and Moderna, could benefit efforts to develop a second-generation malaria vaccine.
“We’ve seen much higher antibody levels from the mRNA vaccines, and they can also be adapted very quickly,” Ghani said, noting that BioNTech recently said it would begin researching a possible malaria shot. “It’s impossible to say how that may affect a malaria vaccine, but we definitely need new options to fight it.”